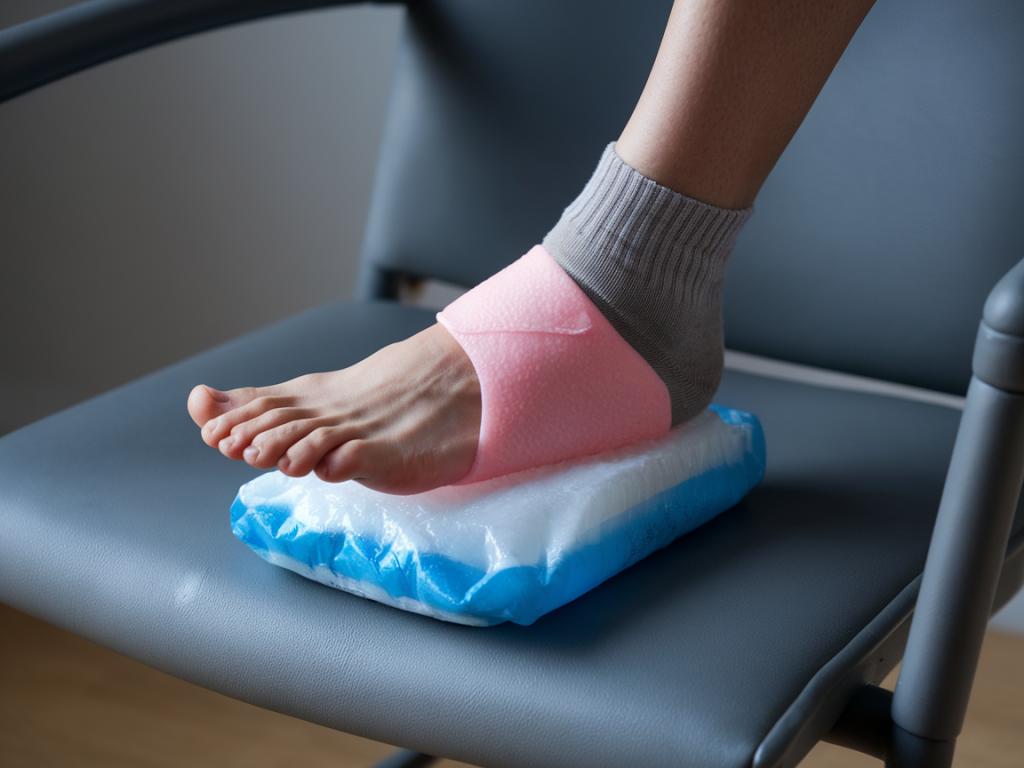
I remember the first time I badly rolled my ankle during a hike — the sharp twinge, the swelling that seemed to appear within minutes, and the uncertainty: what exactly should I do right away to avoid making it worse? Over the years I’ve combined clinical guidance, peer-reviewed recommendations, and practical experience to build a clear, simple plan that I use and recommend for acute foot and ankle sprains. Below is an evidence-based, practical 72-hour approach using cold, compression and elevation (often grouped as the “RICE” or updated “PRICE” principles) to help limit swelling, control pain, and protect tissue while the body starts its repair process.
Why cold, compression and elevation matter in the first 72 hours
Immediately after a sprain, small blood vessels tear, inflammation sets in, and fluid accumulates in the soft tissues. This swelling increases pain and can delay healing by restricting range of motion and increasing tissue stress. The initial 72 hours are important because the inflammatory phase peaks during this time — interventions that safely control swelling and pain can improve comfort and make it easier to progress into gentle movement and rehabilitation.
Cold reduces tissue temperature and nerve conduction speed, which helps with pain and limits blood flow into the injured area. Compression provides an external barrier to fluid build-up. Elevation uses gravity to help drain fluid away from the foot and ankle. Combined, these three are a practical, low-risk way to support early recovery.
Immediate actions (first 0–2 hours)
Right after the injury, my checklist is simple and direct. Quick actions can make a big difference in how much swelling develops.
Structured 72-hour plan
Below I outline a pragmatic schedule you can follow for the first three days. The aim is to control swelling and pain while preventing stiffness and protecting the injured tissues.
| Time frame | Goals | Actions |
|---|---|---|
| 0–24 hours | Limit bleeding and swelling, control pain | |
| 24–48 hours | Maintain swelling control, begin gentle movement | |
| 48–72 hours | Transition toward more active recovery | |
How to apply cold safely and effectively
Cold therapy is most effective when used intermittently — continuous icing risks skin and nerve damage. I recommend:
Practical compression tips
Compression helps limit swelling but must be comfortable and not restrict circulation.
Elevation: small adjustments, big impact
Elevation is simple but underused. When you’re sitting or lying down, aim to keep the foot above the level of the heart. Even small elevations — a pillow under the calf while seated — help. Combine elevation with gentle toe and ankle movements to encourage venous return.
Pain medication and when to use it
I recommend paracetamol or an NSAID (ibuprofen or naproxen) for short-term symptom relief if you have no contraindications. Both can help reduce pain and inflammation; NSAIDs have a stronger anti-inflammatory effect. Use the lowest effective dose and follow product guidance. If in doubt, check with a healthcare provider, especially if you have stomach issues, cardiovascular disease, kidney problems, or are taking other medications.
Red flags and when to see a clinician
Most mild to moderate sprains improve with the 72-hour PRICE approach and then structured rehab. Please seek urgent medical care if you notice:
What comes after 72 hours
By 72 hours you should start focusing more on restoring ROM, balance and strength. Gradual loading of the foot and ankle is important; controlled movement encourages healthy tissue remodeling. Depending on severity, a guided rehabilitation program (even a few sessions with a physiotherapist) can speed recovery and reduce re-injury risk. For persistent pain or instability, imaging or specialist review may be necessary.
If you’d like, I can share simple early rehab exercises you can start after the first 48–72 hours, or a printable checklist to keep near your first-aid kit. Small, consistent steps in the first days after a sprain often determine how quickly and fully you recover — gentle, evidence-based care works.